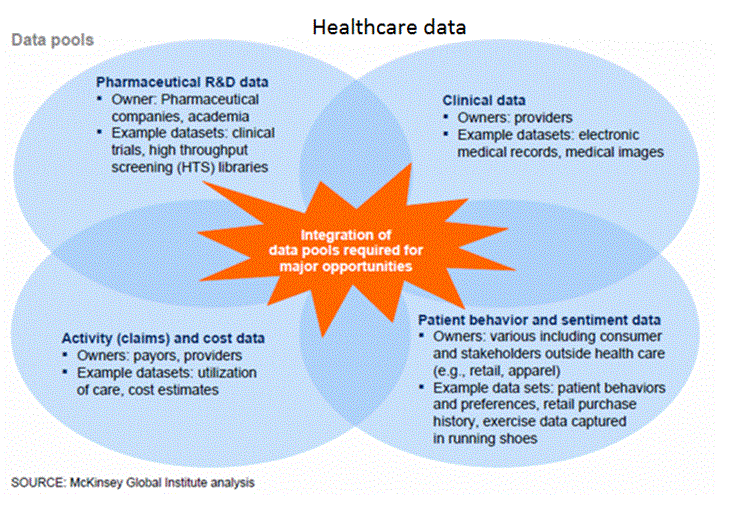
The Information Era has given us the gift of empirical data to study healthcare quality more efficiently. Understanding structure, process and outcomes is understanding how to deliver high quality healthcare. Well, that data is collected and data empowers us to make better decisions. So what’s the problem? Unlike the slide below, data sources are in non-overlapping circles and are only beginning to be integrated in a way to inform decision-making in larger provider organizations. We don’t understand our costs very well. We have no access to aggregated population data for outcomes. We don’t know how the payers analyze our work via their own data. But this is all poised to change: payment reform will incentivize different practices. And by different, I mean in teams. Clinician practices, hospitals, post-acute care facilities like nursing homes and rehab units, insurance companies, pharmaceutical companies or pharmacy benefit management firms… all working together, with integrated data with which to make decisions. This is not an easy task. So how can we pull this off in Western Montana? We need a structure that enables the above and there just so happens to be one that works. I will introduce it here but I will use multiple bits in the future getting you to understand this better. It’s called clinical integration. A clinically integrated network (CIN) is a network of providers (clinics, hospitals, ASC’s, nursing homes, etc.) working together, with protocols and measures mutually agreed upon, to coordinate patient care, improving efficiency, improving quality, decreasing cost, and demonstrating increased value to the market. Okay, that’s a mouthful… How about, “a group of providers working as a team to achieve value” (using that equation for healthcare value again).
The model is quite successful, but at the core is complex IT infrastructure. A CIN depends on interoperability of data systems between different members of the team. Accomplishing it is possible, but a lot of work (engagement) is necessary to pull it off. More on this to come, I promise.